Gastritis: Overview
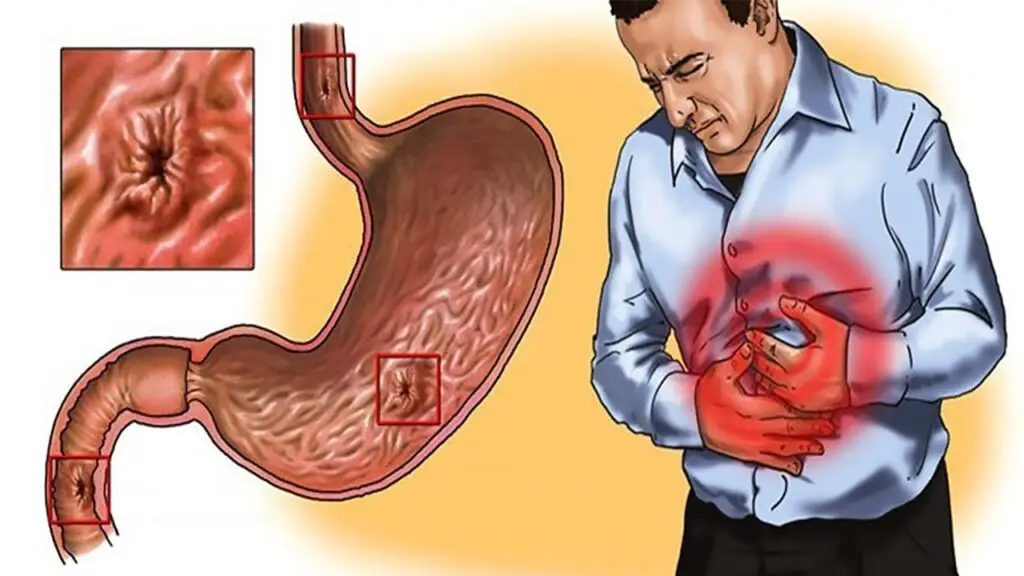
Gastritis is a common clinical term used to describe conditions involving upper abdominal discomfort, indigestion, or dyspepsia, even when specific clinical signs or radiological abnormalities are absent.
[!IMPORTANT] Gastritis is clinically significant due to its potential progression into peptic ulcers or gastric cancer.
Classification
Gastritis is broadly classified into two categories:
- Acute Gastritis: A transient, acute inflammatory involvement of the stomach mucosa.
- Chronic Gastritis: A long-term condition that includes various subtypes.
Types of Gastritis
Acute Gastritis: Overview

Etiopathogenesis
Acute gastritis occurs when the gastric mucosa is injured by various agents. The causes are categorized as follows:
1. Diet and Personal Habits
- Consumption of highly spiced food.
- Excessive alcohol consumption.
- Malnutrition.
- Heavy smoking.
2. Infections
- Bacterial: Helicobacter pylori (most common), Diphtheria, Salmonellosis, Pneumonia, and Staphylococcal food poisoning.
- Viral: Viral hepatitis, Influenza, and Infectious mononucleosis.
3. Drugs
- NSAIDs: Aspirin, Phenylbutazone, Indomethacin.
- Others: Cortisone (steroids), Iron preparations, and Chemotherapeutic agents.
4. Chemical and Physical Agents
- Ingestion of corrosive chemicals (e.g., caustic soda, phenol, lysol).
- Gastric irradiation (radiation therapy).Freezing.
5. Severe Stress
- Emotional factors: Shock, anger, or deep resentment.
- Physical trauma: Extensive burns, major surgery, or severe injury.
Mechanisms of Mucosal Injury
When the agents listed above trigger acute inflammation, they typically do so through one of these three mechanisms:Mechanism Description Ischaemia Reduced blood flow leading to mucosal hypoperfusion. Epithelial Damage Increased acid secretion (often due to H. pylori) that breaks the protective epithelial barrier. Loss of Protection Decreased production of the bicarbonate buffer, which normally neutralizes stomach acid.
Morphology of Acute Gastritis
The morphology (physical changes) of acute gastritis is studied at two levels: what can be seen with the naked eye (Gross) and what is seen under a microscope (Microscopic).
1. Gross Features (Visual Appearance)

- Oedematous Mucosa: The lining of the stomach appears swollen and thick due to fluid accumulation.
- Abundant Mucus: There is a noticeable increase in the production of mucus on the surface.
- Haemorrhagic Spots: Small, red spots or patches are visible, indicating tiny areas of bleeding within the tissue.
2. Microscopic Features (Histology)

The microscopic findings vary depending on the severity and stage of the inflammation:
Oedema: Fluid buildup is present within the tissue layers.
Neutrophil Infiltration: The lamina propria (a thin layer of connective tissue) is heavily infiltrated by neutrophils (acute inflammatory cells).
Acute Haemorrhagic & Erosive Gastritis:
- Sloughing: Parts of the mucosal surface are shed or “sloughed off.”
- Erosions: Shallow loss of the top layer of the mucosa.
- Surface Haemorrhage: Active bleeding is visible on the surface of the gastric lining.
Summary Table
| Feature | Description |
|---|---|
| Mucosa | Swollen (Oedematous) and Red. |
| Secretions | Excess mucus present. |
| Primary Cell Type | Neutrophils in the lamina propria. |
| Severe Cases | Presence of Erosions (surface loss) and Haemorrhage (bleeding). |
Chronic Gastritis: Overview

Chronic gastritis is the most frequent histological finding in gastric biopsies. It is a long-term inflammatory condition with some unique clinical characteristics:
- Clinical Correlation: Symptoms often do not match the severity of the tissue damage. In fact, about 35% of biopsies showing chronic gastritis come from patients whose stomachs appeared normal during an endoscopy.
- Age Factor: Incidence increases with age. The average age for symptomatic patients is 45 years, which is similar to the age group affected by gastric ulcers.
Etiopathogenesis (Causes)
Chronic gastritis can develop from repeated attacks of Acute Gastritis or from the following specific factors:
1. Infections & Associated Diseases
- H. pylori Infection: This is the most common and strongly implicated cause.
- Secondary to Other Conditions: It is often associated with Gastric ulcers, Duodenal ulcers, or Gastric carcinoma.
2. Biological & Chemical Factors
- Duodenal Reflux: Backflow of bile and duodenal contents into the stomach, commonly seen after surgeries near the pylorus.
- Anemia: Chronic hypochromic anemia is frequently linked with the atrophic type of gastritis.
3. Immunological Factors
In cases of Atrophic Gastritis, the body’s immune system may mistakenly attack itself:
- Anti-parietal cell antibodies: Attack the cells that produce stomach acid.
- Anti-intrinsic factor antibodies: Interfere with Vitamin B12 absorption.
Mechanism of Injury
Regardless of the cause, the process follows a specific pathway:
- Cytotoxic Effect: The injurious agent (bacteria, bile, or antibodies) directly attacks the gastric mucosal epithelium.
- Barrier Breakdown: This attack breaks the protective mucosal barrier of the stomach.
- Inflammatory Response: Once the barrier is breached, the body triggers a chronic inflammatory response, leading to permanent tissue changes over time.
Quick Comparison
| Feature | Acute Gastritis | Chronic Gastritis |
|---|---|---|
| Primary Cell | Neutrophils | Lymphocytes & Plasma cells |
| Onset | Sudden/Transient | Gradual/Long-term |
| Endoscopy | Clearly visible (redness/spots) | Often appears normal (35% of cases) |
| Main Cause | NSAIDs, Alcohol, Stress | H. pylori, Autoimmunity, Reflux |
Clinico-Pathologic Classification of Chronic Gastritis
The classification is based on the location of the mucosa affected and the underlying cause.
1. Type A Gastritis (Autoimmune Gastritis)
- Location: Primarily involves the Body and Fundus of the stomach.
- Etiology: Autoimmune; characterized by circulating antibodies against parietal cells and intrinsic factor.
- Pathophysiology:
- Depletion of parietal cells leads to Hypochlorhydria or Achlorhydria (low/no stomach acid).
- Impaired intrinsic factor leads to Pernicious Anaemia (Vitamin B12 deficiency).
Key Feature:
- Often associated with other autoimmune diseases (e.g., Hashimoto’s thyroiditis, Addison’s disease).
- It leads to Hypergastrinaemia because the body tries to compensate for low acid by overproducing Gastrin (G-cell hyperplasia).
2. Type B Gastritis (H. pylori-Related)
- Location: Mainly involves the Antral mucosa.
- Etiology: Non-autoimmune; caused by Helicobacter pylori infection.
- Pathophysiology:
- Known as Hypersecretory Gastritis because it is often associated with excessive acid secretion.
- Frequently linked to the development of Peptic Ulcers.
- Key Feature: This is the most common form specifically related to infection and does not have an autoimmune basis.
3. Type AB Gastritis (Mixed / Environmental / Atrophic)
- Location: Affects both Type A and Type B regions (Body, Fundus, and Antrum).
- Etiology: “Environmental Gastritis,” caused by various unidentified environmental factors.
- Pathophysiology:
- Progresses from Chronic Superficial Gastritis to Chronic Atrophic Gastritis.
- Characterized by Mucosal Atrophy and Metaplasia (tissue changes into intestinal or pseudopyloric types).
- Key Feature: The most common type across all age groups.
Summary Table: Type A vs Type B vs Type AB
| Feature | Type A (Autoimmune) | Type B (H. pylori) | Type AB (Environmental) |
|---|---|---|---|
| Primary Site | Body & Fundus | Antrum | Entire Stomach |
| Common Cause | Autoantibodies | H. pylori infection | Environmental factors |
| Acid Level | Low (Achlorhydria) | High (Hypersecretory) | Variable/Decreasing |
| Associations | Pernicious Anaemia | Peptic Ulcer | Mucosal Atrophy |
| Gastro-Cancer Risk | Increased | Increased | Significantly Increased |
Morphology of Chronic Gastritis
1. Gross Features (Naked Eye)
Unlike acute gastritis, the gross appearance of chronic gastritis is often inconclusive. During endoscopy, the mucosa may appear:
- Normal (most common in early stages).
- Atrophied (thin, pale mucosa with visible underlying blood vessels).
- Oedematous (swollen or reddened).
2. Histological Criteria for Categorization
Pathologists classify chronic gastritis based on three main microscopic factors:
- Depth of Inflammation: Whether it is limited to the surface (superficial) or involves the full thickness of the mucosa (deep).
- Activity Level: Whether the inflammation is Quiescent (inactive) or Active (showing signs of acute-on-chronic inflammation).
- Metaplasia: Presence of Intestinal Metaplasia (stomach lining turning into intestinal-type tissue) or Pseudopyloric Metaplasia.
Morphologic Classification
Based on the criteria above, chronic gastritis is traditionally divided into:
- Chronic Superficial Gastritis: Inflammation is restricted to the upper layer of the mucosa.
- Chronic Atrophic Gastritis: Inflammation extends deeper, leading to the loss of gastric glands.
- Gastric Atrophy: The final stage where glands are significantly lost and the mucosa becomes very thin.
- Chronic Hypertrophic Gastritis (Ménétrier’s Disease): Characterized by giant mucosal folds.
- Uncommon Forms: Specific types like granulomatous or lymphocytic gastritis.
The Sydney System
The Sydney System is the modern, more detailed standard for recording histological changes. It evaluates four key parameters:Parameter Details Included Etiology Identifies the cause (e.g., H. pylori, Autoimmune, NSAIDs). Location Where it is found (Pangastritis, Antral-predominant, or Body-predominant). Morphology Severity/depth of inflammation, presence of atrophy, and metaplasia. Special Features Unusual findings like Granulomas, Eosinophilic infiltration, Necrosis, or Haemorrhage.
Key Takeaway
- The Sydney System is preferred in clinical practice because it combines the cause, location, and microscopic appearance into one complete diagnosis, whereas older classifications focused only on the appearance of the tissue.
1. Chronic Superficial Gastritis
Overview & Histology
- Definition: Inflammation limited to the superficial layer of the gastric mucosa.
- Microscopic Features: The superficial layer shows an inflammatory infiltrate of plasma cells and lymphocytes.
- Key Distinction: The deeper layers, which contain the gastric glands, remain histologically normal.
- Outcome: It may resolve completely or progress into Chronic Atrophic Gastritis.
The Role of Helicobacter pylori
Discovered by Warren and Marshall (Nobel Prize 2005), H. pylori is a spiral-shaped bacterium that thrives in the stomach’s acidic environment.
- Prevalence: Responsible for almost all active cases and about 65% of quiescent (inactive) cases of chronic superficial gastritis.
- Location: The bacteria inhabit the epithelial layer on the luminal surface.
- Note: It does not invade the mucosa.
- Note: It is not seen in areas with intestinal metaplasia.
Diagnostic Techniques for H. pylori
Category Test Type Description Invasive (Biopsy) Histology Uses special stains: Giemsa, Steiner silver, or Warthin-Starry. Biopsy Urease Test Quick and simple, but lower sensitivity. Culture Best for determining antibiotic sensitivity. Non-Invasive Serologic Tests Tests ELISA/Immunoblot (cheap but poor for early follow-up). Urea Breath Test Using C14 urea; highly effective and non-invasive.
Clinical Significance & Risks
While many patients remain asymptomatic, H. pylori is a dangerous long-term resident. It is classified as an independent risk factor for:
- Gastric Adenocarcinoma: Risk increases 3–6 fold.
- MALT Lymphoma: Risk increases 6–50 times.
- Progression: Leads to Chronic Atrophic Gastritis, Gastric Atrophy, and Peptic Ulcer Disease.
Quick Fact: Why "Superficial"?
- It is called “superficial” because the inflammatory cells are like a “blanket” over the top layer.
- As long as the gastric glands below are safe, the stomach can still produce acid and enzymes normally.
- Once the glands are attacked, it becomes Atrophic Gastritis.
2. Chronic Atrophic Gastritis
This stage represents a progression from superficial inflammation to actual tissue destruction.
Core Histological Changes
- Deep Infiltration: Unlike superficial gastritis, the inflammatory cell infiltrate now penetrates the deeper layers of the mucosa.
- Glandular Destruction: There is a progressive loss (atrophy) of epithelial elements, specifically the gastric glands.
- Parietal Cell Loss: These acid-producing cells become very scarce or disappear entirely.
Metaplasia in Atrophic Gastritis
Metaplasia is a process where one adult cell type is replaced by another to better withstand chronic irritation. There are two main types seen here:
I. Intestinal Metaplasia (Most Significant)
This is the most common form and frequently involves the antral mucosa.
Histologic Features:
The stomach lining begins to look like the small intestine. It is characterized by:
- Goblet Cells: Mucus-secreting cells typical of the intestine.
- Paneth Cells and Endocrine Cells: May also appear.
Clinical Significance:
- It is considered a pre-cancerous change. The incidence is particularly high in regions with high gastric cancer rates (e.g., Japan).
- Crucial Note: H. pylori does not colonize areas that have undergone intestinal metaplasia.
II. Pseudopyloric Metaplasia
- Location: Involves the body glands of the stomach.
- Mechanism: The specialized glands in the body are replaced by proliferating mucus neck cells.
- Appearance: These new cells look almost identical to normal pyloric glands (found at the end of the stomach).
- Significance: Its specific clinical significance is currently unknown.
Summary Table: Types of Metaplasia
Feature Intestinal Metaplasia Pseudopyloric Metaplasia Common Site Antrum Body New Cell Type Goblet Cells, Paneth Cells Mucus Neck Cells H. pylori Presence Absent Variable Cancer Risk High (Pre-malignant) Unknown
3. Gastric Atrophy
This is the end-stage of chronic gastritis where the inflammatory process has subsided, leaving permanent structural damage.
- Key Feature: Significant thinning of the gastric mucosa.
- Glandular Loss: There is a complete or near-complete loss of gastric glands.
- Inflammation: Interestingly, active inflammation is absent, though small lymphoid aggregates may still be seen.
4. Chronic Hypertrophic Gastritis (Ménétrier’s Disease)
A rare but clinically significant condition characterized by massive overgrowth of the stomach lining.
- Gross Appearance: The gastric rugal folds (stomach folds) become enormously thickened, resembling the convolutions of the brain (cerebral convolutions).
- Location: Primarily affects the Fundus and Body; it characteristically spares the Antrum.
- Clinical Symptoms: Dyspepsia, vomiting blood (haematemesis), black stools (melaena), and protein-losing enteropathy (leaking of protein from the gut).
- Histology:
- Gastric pits are elongated and tortuous (corkscrew appearance).
- Presence of epithelium-lined cysts in the glandular layer.
- Marked mucosal thickening with parts of the muscularis mucosae extending into the folds.
- Risk: This condition carries an increased risk of gastric cancer.
5. Miscellaneous Forms of Chronic Gastritis
These are specialized types with distinct causes or appearances:Type Key Characteristics Common Cause / Association Eosinophilic Gastritis Thickening of the pyloric antrum with massive eosinophil infiltration in all wall layers. Likely an allergic basis. Chronic Follicular Gastritis A variant of atrophic gastritis featuring numerous lymphoid follicles in the mucosa and submucosa. Often seen in persistent H. pylori infections. Haemorrhagic (Erosive) Gastritis Presence of superficial erosions and mucosal bleeding, often causing severe haematemesis. NSAIDs, bile reflux, or portal hypertension. Granulomatous Gastritis Formation of granulomas (organized clusters of immune cells) in the mucosa. Tuberculosis, Sarcoidosis, Crohn’s disease, or foreign material.
Final Summary Checklist for Gastritis
- Acute: Neutrophils, sudden, usually drug/alcohol-related.
- Type A: Autoimmune, Body/Fundus, Pernicious Anemia.
- Type B: H. pylori, Antrum, Ulcer risk.
- Type AB: Environmental, most common, progression to Atrophy.
- Ménétrier’s: “Brain-like” folds, protein loss, cancer risk.
Frequently Asked Questions (FAQ)
1. What is the main difference between Type A and Type B Gastritis?
Type A gastritis is an autoimmune condition that primarily attacks the body and fundus of the stomach, often leading to Pernicious Anaemia. Type B gastritis is the most common form, caused by H. pylori infection, and typically affects the antrum.
2. Can Gastritis lead to cancer?
Yes, chronic forms of gastritis are significant risk factors for malignancy. H. pylori infection is considered an independent risk factor, increasing the risk of gastric adenocarcinoma by 3–6 fold and MALT lymphoma by up to 50 times. Chronic atrophic gastritis with intestinal metaplasia also shows a high correlation with gastric cancer.
3. What causes Acute Gastritis to flare up?
Acute gastritis is often a transient reaction to irritants such as highly spiced food, excessive alcohol, heavy smoking, or the use of NSAIDs like Aspirin and Ibuprofen. Severe emotional stress or physical trauma can also trigger the condition.
